
Telemedicine is no longer a temporary digital add-on. In 2026, it is part of the core healthcare infrastructure that shapes patient access, provider workflows, operational efficiency, and long-term scalability. That shift has raised the stakes for healthcare organizations. Choosing a technology partner for telemedicine software development now means evaluating how a platform supports scheduling, documentation, billing, remote monitoring, integrations, compliance, and future growth.
This guide breaks down what modern telemedicine software should include, when custom development creates a strategic advantage, and where projects most often go wrong. It also covers broader topics like security, interoperability, and total cost of ownership (TCO) for telehealth software.
If you are assessing a new telemedicine platform or rethinking an existing one, this article will help you make that decision on firmer operational and technical ground.
Why telemedicine platform development efforts matter more in 2026 than they did in 2020?

Telemedicine software has moved far beyond its initial role as an emergency response during the pandemic. Today, it is a strategic infrastructure decision that directly affects how healthcare organizations deliver care, scale operations, and remain competitive. Unlike the early 2020s when speed of deployment was the priority, organizations today must evaluate telemedicine software platforms based on long-term performance, integration, and sustainability.
Virtual care has moved from experimentation to infrastructure
Telemedicine software has evolved from a simple pandemic-era measure and has become embedded in the core healthcare infrastructure, as reflected in the surge in adoption: in 2024, 71.4% of physicians reported using telehealth in their practices weekly, compared to 25.1% in 2018.
There are a few reasons why more and more healthcare organizations invest in software for telehealth:
- Rising chronic disease burden. Chronic conditions such as diabetes, cardiovascular disease, and respiratory disorders require continuous monitoring rather than episodic care. Traditional in-person models are not designed to support this level of ongoing interaction. Telemedicine platforms, especially when combined with remote patient monitoring (RPM), allow providers to track patient data in real time, intervene earlier, and reduce hospital readmissions.
- Digital-first patient expectations. Patients increasingly expect healthcare to be accessible on demand, mobile-friendly, and frictionless, like other mobile services. Appointment scheduling, communication, and follow-ups are now expected to happen online, with minimal effort. Custom telehealth software solutions must therefore deliver consumer-grade user experiences, including fast onboarding, intuitive navigation, and reliable performance.
- Healthcare workforce shortages. Global shortages of physicians, nurses, and support staff are forcing healthcare organizations to increase efficiency without compromising the quality of care. Telemedicine software helps extend provider capacity by enabling shorter consultations, asynchronous communication, and better triage. It also reduces administrative overhead through automation and centralized workflows.
The market is entering a scale phase
Many healthcare organizations have already implemented telemedicine software for providers at a basic level and are now facing the next set of challenges in scaling it across the entire organizational infrastructure.
Early-stage platforms were typically designed to provide video consultations with little additional functions. Today, organizations are expanding telemedicine across specialties, patient groups, and care pathways.
This creates a new scope of requirements for modern telehealth software solutions, such as:
- The ability to support high patient volumes without performance deterioration. This includes handling simultaneous video sessions, real-time data exchange, and concurrent access by clinicians, patients, and administrative staff. Poorly designed systems often fail under load, leading to dropped consultations, latency issues, and disrupted workflows. Scalable telemedicine platforms rely on cloud-native architecture, load balancing, and real-time monitoring to ensure consistent performance.
- Multi-service digital care models. Remote patient care is no longer limited to one type of visit. Healthcare organizations are expanding into integrated digital care ecosystems that include primary care, mental health services, chronic disease management, follow-ups, and preventive care. Each of these services has different workflow requirements, documentation needs, and compliance considerations. A modern telemedicine platform must support modular workflows, allowing organizations to adapt the system to different specialties without rebuilding core functionality.
- Integration with broader digital health ecosystems. This includes integration with EHR/EMR systems, billing and claims processing tools, pharmacy networks, identity management systems, and remote patient monitoring devices. A robust healthcare interoperability strategy helps to avoid data silos, duplicate work, and compliance risks. As a result, integration capability is often the single most important factor determining long-term platform success.
The main reasons why modern telemedicine platforms turn into ecosystem-based software solutions
First versions of telemedicine software for providers were often implemented quickly, with a narrow focus on enabling remote consultations. As organizations scale their digital care offerings, these limitations become increasingly visible, turning initial solutions into bottlenecks.
Early telemedicine video conferencing software is insufficient for modern healthcare workflows
Many previously developed telemedicine platforms were built around a single core feature: video visits. While this was sufficient during the initial adoption phase, it quickly proved inadequate for long-term use.
Modern telemedicine software development is centered around a full range of healthcare workflows, including:
- Scheduling. Telemedicine platforms must handle complex scheduling scenarios, including multi-provider availability, time zone differences, automated reminders, and integration with existing appointment systems. Advanced scheduling also includes triage-based booking, where patients are routed to the appropriate provider based on symptoms or urgency.
- Clinical documentation. Providers need to document visits efficiently without duplicating work. This requires structured templates, real-time note-taking, and seamless integration with EHR systems. Without this, clinicians are forced to switch between systems, increasing administrative burden and reducing productivity.
- Billing and coding. A white-label telemedicine platform needs to support Current Procedural Terminology (CPT) coding, insurance verification, claims submission, and reimbursement workflows. Incomplete billing integration often leads to revenue leakage and compliance risks.
- Patient monitoring. Telemedicine increasingly includes remote patient monitoring (RPM), allowing providers to track vital signs and health metrics between visits. This requires integration with wearable devices, alert systems for abnormal readings, and dashboards for continuous patient oversight.
- Analytics and reporting. Healthcare organizations need visibility into performance metrics such as visit volume, patient outcomes, provider efficiency, and revenue. Telemedicine software must provide built-in analytics or integrate with reporting systems to support data-driven decision-making.
Learn how CPT software solutions help to manage healthcare revenue cycles, prevent billing errors, and increase processing speed and claim management. Read more about it!
Telemedicine software usage is stabilizing, but remains widespread
Telehealth software adoption has moved past its rapid growth phase and is now stabilizing at a consistently high level. Recent data confirms this transition: as of 2025, 54% of Americans have had a telehealth visit. This shift is important: it signals that telehealth is now driven by sustained demand and habitual use.
As usage stabilizes, telemedicine becomes one of the core channels for patient interaction, alongside in-person care. This means platforms must deliver consistent performance across scheduling, consultations, and follow-ups. Any friction in the experience directly impacts patient retention.
The implication is clear: software for telehealth is no longer an experimental service. It is a standard touchpoint in the patient journey, and platforms must be built to support it at scale.
Patient satisfaction remains extremely high
While adoption has stabilized, patient satisfaction with telemedicine remains consistently strong. Data shows that 89% of telehealth users report satisfaction with their most recent virtual visit.
This level of satisfaction highlights that patients value telemedicine for its convenience, accessibility, and time efficiency. However, it also shifts the competitive landscape. When baseline satisfaction is already high, differentiation no longer comes from offering telemedicine itself, but from how well the experience is delivered.
For healthcare organizations, this means building stable, scalable software that supports patient engagement through smooth, reliable, and intuitive interactions. Poor scheduling flows, unreliable connections, or fragmented communication can quickly erode trust, even if the concept of telehealth remains appealing.
Buy vs build: How healthcare organizations should approach telemedicine software development in 2026
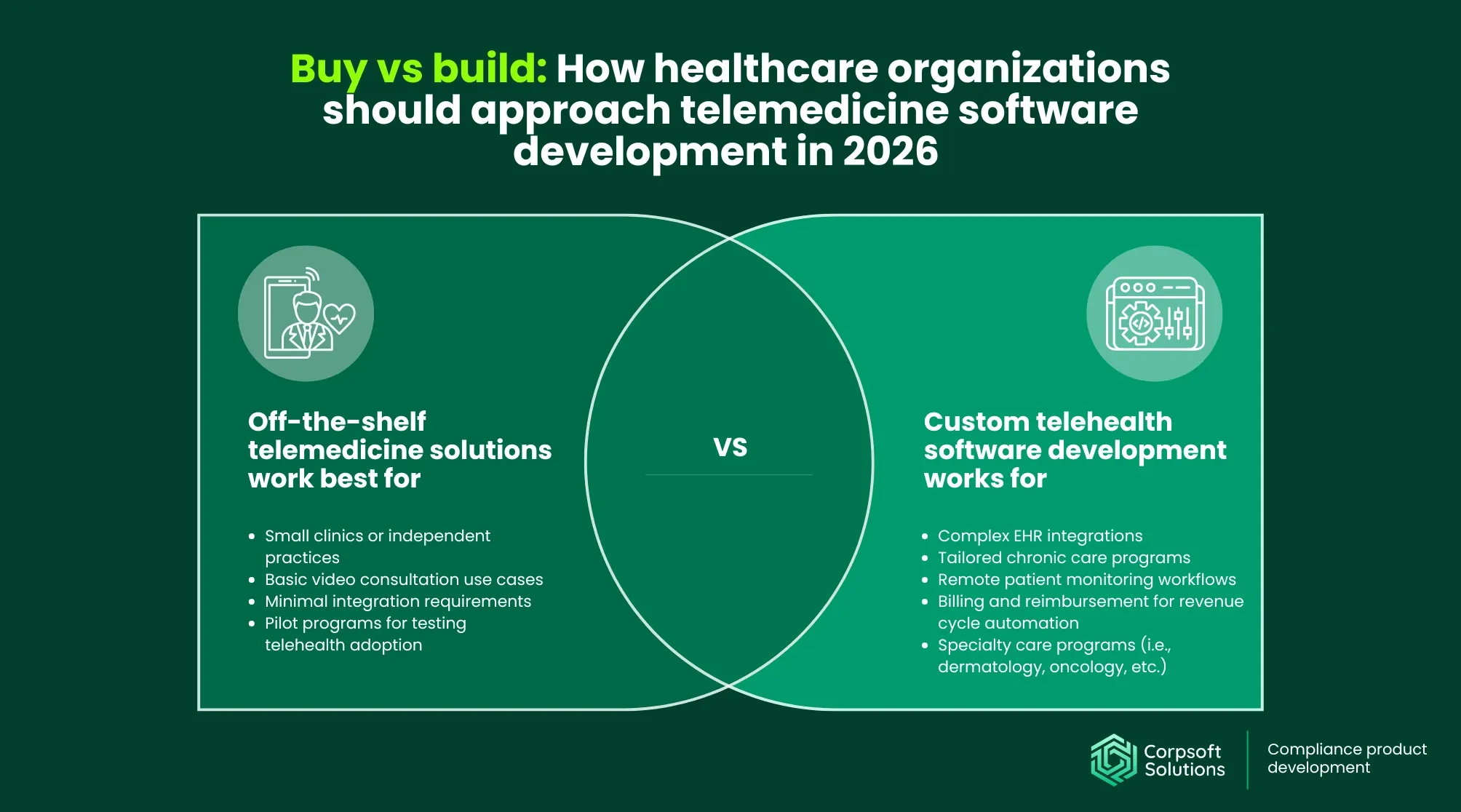
Choosing between off-the-shelf telemedicine software and custom development can make or break your success. Companies need to consider the scalability, operational efficiency, and long-term costs of the final product, and evaluate how well their platform will support complex workflows, integrations, and future growth.
When off-the-shelf telemedicine software works
Out-of-the-box software for telemedicine is most effective when simplicity and speed are the primary goals. It’s typically suitable for:
- Small clinics or independent practices with limited IT resources
- Basic video consultation use cases without complex workflows
- Minimal integration requirements, where systems can operate in isolation
- Pilot programs, where organizations are testing telemedicine adoption
These platforms offer faster deployment and lower upfront costs. However, they often come with limitations in customization, scalability, and integration. As organizations grow, these constraints can become critical bottlenecks.
When custom telehealth software development creates a competitive advantage
Custom telemedicine software development becomes the preferred option when telemedicine is deeply embedded into clinical and operational processes. Healthcare organizations should consider custom solutions when telemedicine touches:
- EHR workflows. Outdated EHR/EMR systems can easily become barriers to seamless integration. Legacy compatibility issues can result in duplicating documentation across systems, increasing administrative burden and risk of errors. Custom development allows organizations to design workflows in which telemedicine interactions are fully embedded in clinical records, rather than treated as separate processes.
- Chronic care programs. Chronic disease management requires continuous patient engagement, and off-the-shelf systems rarely support personalized care plans, alerts for abnormal readings, and coordinated follow-ups. accommodate the complexity of longitudinal care. Custom solutions, by contrast, can align with value-based care models and patient-specific treatment pathways.
- Remote patient monitoring (RPM). RPM introduces additional technical requirements, including integration with wearable devices, real-time data ingestion, and automated alerting. Custom telehealth software development enables flexible data pipelines, device integrations, and condition-specific dashboards, which are difficult to achieve with generic solutions.
- Revenue cycle automation. Telemedicine services must be tightly aligned with billing and reimbursement workflows. This includes CPT coding, insurance verification, claims submission, and payer-specific rules. Custom platforms can automate these workflows and ensure that telemedicine services are properly captured within the broader revenue cycle.
- Specialty care pathways. Different healthcare specialities may have fundamentally different software requirements. Some, such as dermatology, rely heavily on image-based diagnostics, while mental health requires session continuity and secure communication. Custom solutions allow organizations to build specialty-specific interfaces, workflows, and data structures, ensuring that the platform supports clinical needs rather than forcing providers into generic processes.
Explore how Corpsoft Solutions’ team developed a HIPAA-compliant teledermatology solution that reduced patient wait times by 4x and improved diagnostic speed by 1.5x!
The decision framework healthcare leaders actually use
Selecting the best telemedicine platform development company is critical to achieving successful outcomes. Healthcare organizations should evaluate vendors across key dimensions:
|
Evaluation area |
Key question |
| Integration experience | Which EHR systems have you integrated with? |
| Compliance | How do you ensure HIPAA compliance? What other regulations do you cover? |
| Interoperability | What standards and approaches do you use (FHIR, HL7)? |
| Scalability | How do you support large patient volumes and system growth? |
| Healthcare expertise | What relevant healthcare projects have you delivered? |
| Delivery model | What does your implementation roadmap look like? |
Vendor evaluation: Green flags vs red flags
Choosing a telemedicine vendor is about identifying possible risks before throwing money into production. In practice, the difference between a successful implementation and a failed one often comes down to how clearly a vendor can explain compliance, integrations, and delivery. The table below highlights common green flags and red flags to look for during vendor evaluation.
| Pros |
Cons |
| Clear compliance framework Defined interoperability strategyDemonstrated healthcare domain expertise Realistic implementation roadmaps Capability for a long-term partnership |
Vague compliance claims Unclear integration strategy Lack of healthcare domain expertise Unrealistic implementation timelines No post-launch support or scalability plan |
In practice, the decision is rarely binary. Many organizations adopt a hybrid approach, combining off-the-shelf components with custom telemedicine software development to balance speed and flexibility.
The key is to choose a partner that can align technology with healthcare workflows, not just deliver features.
Technical foundations of telemedicine software development: system architecture explained

Modern HIPAA-compliant telehealth software is a multi-layered, distributed system designed to support clinical workflows, real-time communication, and secure data exchange. Understanding its architecture is essential for evaluating scalability, integration readiness, and long-term sustainability. At a high level, telemedicine system architecture consists of several interconnected layers:
- Presentation layer (interfaces). This is the outermost layer of the system architecture, which includes patient- and provider-facing applications, such as mobile apps, web portals, and admin dashboards. Interfaces handle appointment booking, video consultations, messaging, and access to medical data. The key requirement here is usability and performance, as this layer directly impacts patient experience and clinician adoption.
- Application layer (core functionality). This is the operational core of the telehealth platform. It includes modules like video conferencing, scheduling engines, messaging systems, clinical documentation tools, billing, and payment processing. These components define how telemedicine workflows function. A well-designed application layer ensures that all processes are cohesive and efficient.
- Integration layer (interoperability). The integration layer connects the telemedicine platform to external systems, including EHR/EMR systems, pharmacy networks, third-party administrators for billing and claims management, identity providers, and remote patient monitoring devices. This layer typically relies on standards like FHIR or HL7 and includes APIs, middleware, and data transformation logic.
- Data and analytics layer. This layer manages patient records, consultation data, system logs, and organizational performance metrics. It also supports analytics and reporting, enabling healthcare organizations to track patient outcomes and operational efficiency. A robust data layer is essential for decision-making, compliance, and scaling care delivery.
- Security and compliance layer. Security is embedded across all layers, but it is often treated as a separate architectural concern. This layer ensures that the platform complies with HIPAA, GDPR, and other regulatory requirements while protecting sensitive patient data.
Most telemedicine software development failures are not caused by missing features, but by poor architectural decisions, especially around integrations and scalability. A well-structured system allows healthcare organizations to expand services without rebuilding the platform and maintain compliance as regulations evolve.
Essential features of modern telemedicine software
Modern telemedicine software development services must go beyond basic video functionality and support end-to-end care delivery workflows. This means enabling seamless interactions for both patients and providers while ensuring that clinical, administrative, and financial processes are fully integrated.
Patient-facing capabilities

From the patient’s perspective, telemedicine software must provide a frictionless, intuitive, and reliable experience across the entire care journey: from booking to follow-up. Below is a comprehensive set of core patient-facing features:
- Self-scheduling. Patients should be able to book appointments based on real-time provider availability, reducing administrative friction and improving access to care.
- Remote visit access. This feature helps patients to join consultations easily from the web or mobile devices without complex setup, ensuring accessibility across different user groups.
- Digital intake forms. By collecting medical history, symptoms, and consent forms before the visit, healthcare providers can streamline consultations and reduce time spent on administrative tasks.
- Asynchronous messaging. Establishing communication between patients and providers outside of live visits, as well as enabling follow-ups, clarifications, and ongoing engagement, helps to create a positive patient experience.
- Digital prescriptions (eRx). This workflow helps providers to send prescriptions directly to pharmacies, improving convenience and reducing treatment delays.
- Payment integration. Online payment integration, insurance processing, and transparent billing make financial interactions simple and predictable.
- Automated reminders and notifications. Alerts about appointment confirmations, reminders, and follow-up notifications that help to reduce no-shows and improve patient adherence.
- Patient portal access. Centralized access to visit summaries, prescriptions, lab results, and communication history improves transparency and patient engagement.
- Multi-device compatibility. Ensures consistent experience across smartphones, tablets, and desktops, accommodating different user preferences and technical capabilities.
- Secure authentication and identity verification. Protects patient data through login systems, multi-factor authentication, and identity checks, ensuring privacy and compliance.
- Multilingual support. Expands accessibility by allowing patients to interact with the platform in their preferred language, which is critical for diverse populations.
- Accessibility features. Screen reader compatibility, adjustable text sizes, and simplified navigation controls to support elderly users and patients with disabilities.
- Post-visit summaries and care instructions. Provides patients with clear next steps, treatment plans, and follow-up guidance, improving adherence and outcomes.
These capabilities ensure that telemedicine software for clinics delivers a consumer-grade experience, which is essential for patient adoption, retention, and long-term engagement.
Clinician-facing functionality

Unlike patient-facing features, telemedicine software for providers must prioritize efficiency, accuracy, and seamless workflow integration. Clinician-facing functionality must reduce cognitive load and administrative burden while ensuring that care delivery remains consistent and compliant.
Key capabilities include:
- Contextual EHR access. Telehealth software should enable clinicians to view patient history, lab results, medications, and prior visits directly within the telemedicine interface, eliminating the need to switch between systems and ensuring continuity of care.
- Structured visit documentation. A telemedicine platform should include standardized templates and forms to capture clinical data during consultations, improving accuracy, consistency, and compliance while reducing manual effort.
- Clinical decision support. This functionality assists clinicians in providing evidence-based recommendations, alerts, and guidelines during consultations, enabling more informed decision-making and the identification of potential risks.
- Referral workflows. Shared patient records and coordinated follow-ups facilitate seamless referrals to specialists and multi-department cooperation, ensuring continuity across different levels of care.
- Multi-participant visits. Another tool for the collaborative care model that allows multiple providers, caregivers, or interpreters to join the same consultation in more complex clinical scenarios.
- Care team collaboration. Efficient communication between healthcare professionals through shared notes, messaging, or task management improves coordination and reduces fragmentation of care.
These features ensure that telemedicine platforms for clinics integrate naturally into clinical workflows, allowing providers to deliver care efficiently without adding unnecessary complexity or administrative overhead.
Remote patient monitoring is a new healthcare standard
Remote patient monitoring (RPM) is rapidly becoming a core component of telemedicine, particularly for managing chronic conditions such as diabetes, hypertension, and cardiovascular disease. Instead of relying on periodic in-person visits, providers can continuously track patient health data and intervene early when risks are detected.
This shift is closely tied to the growing adoption of medical IoT (mIoT) and wearable devices, such as smartwatches, glucose monitors, and connected blood pressure cuffs. Recent data show wearable device adoption increased to 36.36% in 2022, up from 28%-30% in 2019. These devices generate real-time health data that can be transmitted directly to telemedicine platforms, enabling ongoing monitoring outside clinical settings.
As a result, RPM supports a transition from reactive to proactive and preventive care, improving patient outcomes while reducing hospital readmissions.
Learn how we developed a HIPAA-compliant telemedicine platform for vision screening that uses eye pathology tests, which patients can access from their laptops or mobile devices.
Ways in which AI can shape modern telemedicine software development
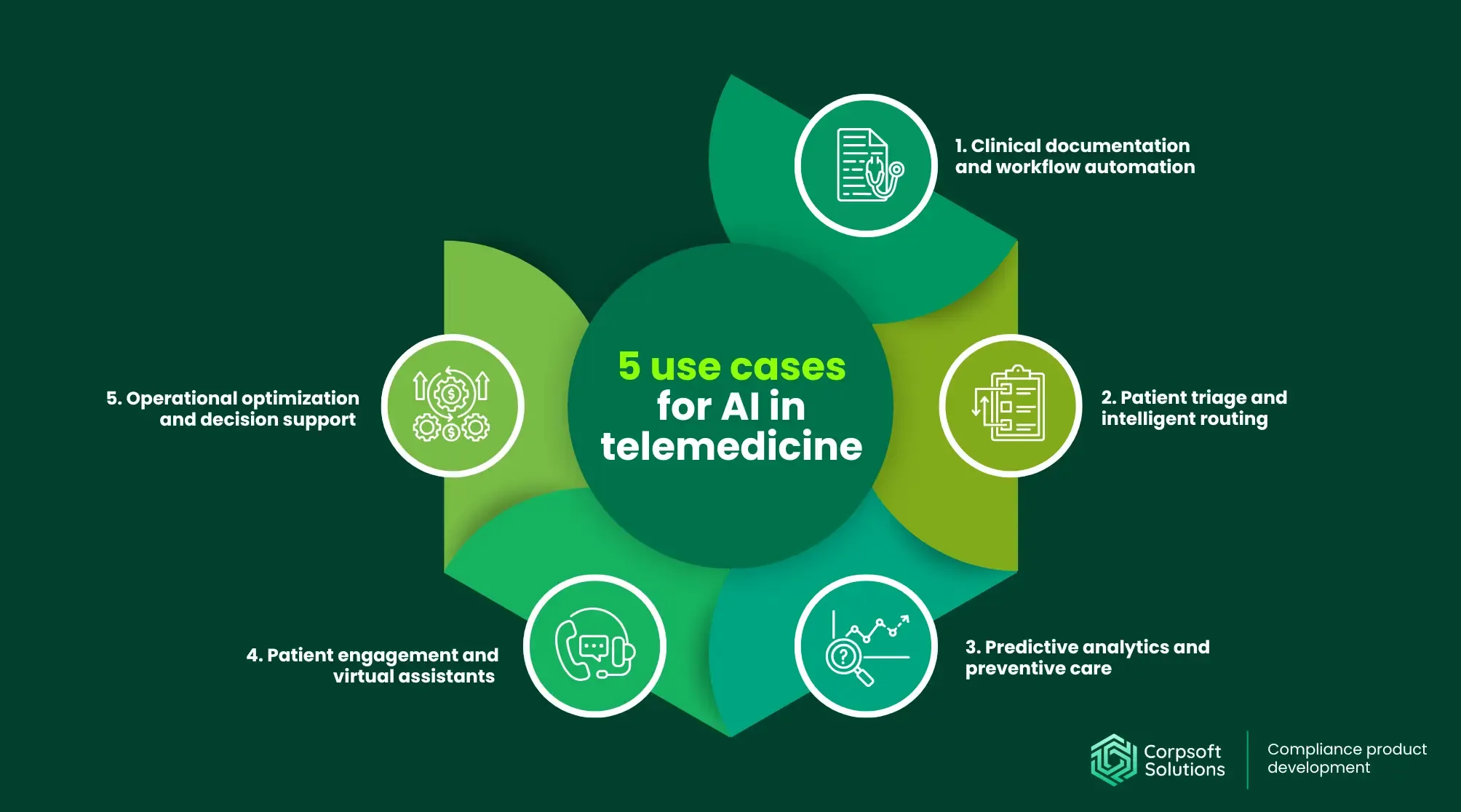
Artificial intelligence is rapidly becoming a core layer of telemedicine platforms, transforming them from tools that enable remote consultations into systems that actively optimize workflows, support clinical decisions, and enable proactive care delivery. AI adoption in healthcare grew to 85% of organizations by the end of 2024, with 82% reporting measurable ROI.
These numbers highlight that AI in telemedicine is becoming a core enabler of scalable digital care models and can have the greatest impact in situations that require processing large volumes of data and making quick decisions, such as:
- Clinical documentation and workflow automation. AI-powered workflow automation tools can automatically transcribe consultations in real time and extract structured medical data. This reduces administrative burden, which can consume a large share of clinician time. As a result, telemedicine platforms are increasingly designed to minimize manual input and standardize documentation.
- Patient triage and intelligent routing. AI-powered triage improves resource allocation and reduces wait times, especially in high-demand environments. In some emerging models, AI-assisted systems are already showing high diagnostic alignment with clinicians (over 80%) in telehealth scenarios.
- Predictive analytics and preventive care. AI systems can detect early risk signals and trigger interventions. Core applications like remote monitoring and predictive analytics are improving both patient engagement and operational effectiveness. This is particularly important for chronic disease management, where early intervention reduces complications and costs.
- Patient engagement and virtual assistants. Some medical practices already use AI chatbots or virtual assistants for increasing patient engagement, with rapid expansion expected. These tools are especially valuable for scaling communication without increasing staff workload.
- Operational optimization and decision support. By analyzing system logs and user behavior, AI agents in healthcare can detect patterns such as delayed consultations, repeated manual steps, or bottlenecks in documentation and billing processes. These insights help organizations streamline workflows, eliminate redundancies, and reduce administrative overhead.
Integration complexity: the hidden risk in telemedicine software development

Integration is one of the most underestimated challenges in telemedicine app development. While features like video visits or messaging are relatively straightforward to implement, the real complexity lies in connecting the platform to existing healthcare systems. In practice, integration is often the primary source of delays, cost overruns, and long-term technical debt.
Telemedicine platforms rarely operate independently
Successful telemedicine solutions must function as part of a broader healthcare ecosystem. This requires integration with:
- EHR/EMR systems
- patient portals
- payment gateways
- pharmacy networks
- identity providers
- medical devices
- billing and claims management
- reporting and analytics
- notifications and alerts
Each of these integrations introduces its own APIs, data models, and compliance requirements, making the system architecture significantly more complex and increasing the importance of a well-designed integration strategy.
Interoperability maturity is improving, but still uneven
Although interoperability standards such as FHIR and HL7 have improved data exchange capabilities, real-world implementation remains inconsistent. Many healthcare organizations still rely on legacy systems with limited or proprietary APIs, which complicates integration efforts.
As a result, telehealth software providers often face challenges with:
- inconsistent data formats
- partial or unreliable system connectivity
- complex data reconciliation processes
This gap between theoretical interoperability and practical implementation is a key reason why telemedicine projects encounter unexpected difficulties.
Corpsoft Solutions’ recommendations for addressing the most common development and integration issues with telehealth platforms
Telemedicine software development and integration issues typically manifest in operational problems that directly impact care delivery and revenue. Below, you’ll find the most common issues that arise during the telehealth software development, integration, and maintenance stages, along with our tips on how to address them, backed by Corpsoft Solutions’ expertise in building healthcare products.
| Issue | Project stage | Why does it happen? | Business impact | Corpsoft Solutions’ recommendations |
| Incorrect patient identity matching | Integration | Lack of unified patient identifiers, inconsistent data across systems | Clinical errors, patient safety risks, and fragmented records | Implement Master Patient Index (MPI), use deterministic + probabilistic matching, and enforce data validation |
| Broken billing workflows | Integration / Maintenance | Misalignment with payer requirements, incomplete CPT mapping | Revenue leakage, claim denials, and delayed reimbursements | Integrate billing early, validate with payers, automate coding, and eligibility checks |
| Clinical data synchronization issues | Integration | Asynchronous systems, unreliable APIs | Incomplete patient data, delayed decisions, and clinician frustration | Use event-driven architecture, retry mechanisms, and consistency checks |
| Duplicate documentation | Development / Integration | Lack of EHR integration, parallel workflows | Increased admin workload, clinician burnout, inefficiency | Enable EHR write-back, unify workflows, and eliminate redundant systems |
| API instability or limitations | Integration / Maintenance | Legacy systems, poorly documented APIs | System downtime, failed integrations, delayed feature delivery | Use middleware, abstraction layers, and continuous API monitoring |
| Performance degradation under load | Development / Maintenance | Poor scalability planning, limited infrastructure | Dropped calls, poor patient experience, lost revenue | Implement cloud scaling, load balancing, and stress testing |
| Security gaps in integrations | Integration / Maintenance | Weak third-party compliance, insufficient controls | Data breaches, regulatory fines, reputational damage | Conduct security audits, enforce encryption, and ensure vendor compliance (BAA, GDPR, etc.) |
| Data format inconsistencies | Integration | Different standards (FHIR, HL7, proprietary formats) | Data errors, failed interoperability, and reporting inaccuracies | Implement transformation layers, standardize data models |
| Notification failures and delays | Maintenance | Reliance on third-party messaging, no redundancy | Missed appointments, reduced engagement, patient dissatisfaction | Use multi-channel alerts, delivery monitoring, and failover systems |
Security and compliance requirements for telemedicine platforms
Security and compliance are foundational to telemedicine software development, but HIPAA alone is not sufficient. Healthcare organizations operating across regions or integrating advanced technologies must also consider additional regulatory frameworks, such as:
- US Food and Drug Administration (FDA): for integrating telemedicine platforms with regulated medical devices (e.g., connected ECG monitors or insulin pumps), ensuring safety and clinical reliability
- General Data Protection Regulation (GDPR): when serving patients in the EU, governing how personal health data is collected, processed, and stored. At the
- ISO standards such as ISO 27001 (information security management) and ISO 27799 (health informatics security) outline best practices for protecting sensitive medical data and building secure systems at scale.
Telemedicine security must extend beyond HIPAA checkboxes
Meeting compliance requirements is only the baseline. Telehealth software providers must implement robust, operational security controls, including:
- End-to-end encryption. Allowing data encryption in rest and in transit ensures that patient data remains protected, especially during video consultations and messaging.
- Role-based access control (RBAC). Restricting system access based on user roles prevents unauthorized exposure of sensitive information.
- Secure data storage. Centralized data storage protects medical records through encryption and controlled access policies.
- Audit logging. Audit logs help to track all system activity, enabling traceability and supporting compliance audits.
- Incident response processes. This is essential to define how organizations detect, respond to, and recover from security incidents or breaches.
- Legacy system risk evaluation. Assessing existing healthcare infrastructure (e.g., outdated EHRs, unsupported APIs, legacy databases) helps minimize security vulnerabilities, integration risks, and compliance gaps.
Security risk grows as digital health ecosystems expand
As HIPAA-compliant telemedicine software evolves, it increasingly connects to external systems, expanding the attack surface. Examples of these systems include
- Wearable devices. Smartwatches that track heart rate and activity (Apple Watch, Fitbit), continuous glucose monitors like Dexcom, and connected blood pressure monitors for home use. These devices continuously collect and transmit sensitive health data to telemedicine platforms. If data transmission is not properly secured, it can expose patient information or introduce inaccurate readings into clinical workflows.
- IoT medical devices. Connected devices such as ECG monitors, insulin pumps, and remote cardiac telemetry systems are often integrated into telemedicine platforms for real-time monitoring. These devices may operate on proprietary protocols or outdated firmware, creating vulnerabilities if they are not regularly updated or properly authenticated within the system.
- External analytics systems. A white-label telemedicine platform frequently integrates with BI tools (e.g., Power BI, Tableau) or AI-driven analytics engines to support reporting and decision-making. These systems often require access to large volumes of patient data, increasing the risk of unauthorized access if permissions, data anonymization, or access controls are not properly configured.
These integrations create new security challenges. Each additional connection introduces potential entry points for unauthorized access, data leakage, or system compromise. As a result, a telemedicine app development company must treat telemedicine security as an ecosystem-level responsibility, ensuring that every connected component adheres to consistent security and compliance standards.
Positive user experience as a new outcome in the telehealth software development
User experience (UX) has become a critical success factor in telemedicine platform development, directly influencing adoption, retention, and clinical outcomes. Increasingly, research shows that usability is the primary barrier to digital health adoption.
This issue is particularly visible among older patients, who represent a key telehealth demographic. Studies show that usability challenges are linked to visual, cognitive, and motor limitations, as well as confusing interface design and a lack of clarity in workflows. These factors significantly slow adoption and reduce engagement, especially when platforms are not adapted to real user needs.
More broadly, research reframes the “digital divide” in healthcare as a usability divide, where adoption is limited not by access to technology, but by how intuitive and accessible that technology is.
At the same time, patient trust has become a core component of UX design. Patients expect transparency, reliability, and control over their data. This translates into concrete product requirements such as clear consent flows, visible security indicators, and consistent system performance.
As a result, telemedicine UX shifts from simple interface design guidelines to accessible design solutions that work across diverse patient populations. Compliance with standards such as Web Content Accessibility Guidelines (WCAG) ensures that interfaces are usable for people with visual, auditory, or cognitive impairments,
Total cost of ownership of telemedicine platform development
Total cost of ownership (TCO) in telemedicine software development refers to the full lifecycle cost of building, implementing, operating, and evolving a platform, typically measured over a 3–5-year horizon. Unlike upfront pricing, TCO accounts for all direct and indirect expenses that impact long-term financial performance. For healthcare organizations, understanding TCO is critical because telemedicine platforms are continuously evolving systems tightly integrated into clinical and operational workflows. And here are two most common misconceptions about TCO we’re ready to debunk.
#1 Software licensing is rarely the highest cost
While licensing or initial telemedicine platform cost are often the most visible, they rarely represent the majority of total expenses. Telemedicine platforms require significant investment through different development stages, such as:
- infrastructure setup or adaptation
- integration with existing systems (EHR, billing, devices)
- ongoing maintenance and updates
- scaling infrastructure to support higher patient volumes
- implementing security and compliance measures
Over time, feature development — adding remote monitoring, AI capabilities, or new care pathways — can further increase total costs.
#2 Companies often overlook or underestimate certain expenses
Many healthcare organizations underestimate the cost of operational complexity. Hidden or underestimated expenses often include:
- Compliance audits and security assessments are required to maintain regulatory alignment
- Data migration, especially when replacing legacy systems or consolidating platforms
- Integration maintenance, as external systems update APIs or change requirements
- Customization of analytics and reporting dashboards is needed for performance tracking and decision-making
- Vendor switching or lock-in costs, including data extraction, reimplementation, and retraining staff
These factors can significantly impact long-term budgets if not accounted for early. As a result, organizations should evaluate telemedicine investments not based on initial pricing alone, but on their ability to deliver sustainable value over time.
Learn how to reduce costs for healthcare operations without lowering the quality of patient care with our comprehensive guide to healthcare cost optimization!
Modelling the TCO of telehealth software development for a healthcare organization: a 36-month timeframe
A 36-month timeframe is commonly used when modeling the TCO for telemedicine platforms, as it reflects how these systems are actually planned, deployed, and evolved in real-world healthcare environments. There are several practical reasons for choosing this horizon.
- Development and vendor contracts in healthcare typically span around three years, making it a natural financial and operational planning cycle.
- Most telemedicine platforms begin to require significant updates or architectural improvements within this time period, whether due to scaling needs, regulatory changes, or the addition of new capabilities such as remote patient monitoring or AI-driven features.
- A three-year window provides enough time for organizations to clearly understand and quantify ongoing operational costs, including integration maintenance, infrastructure usage (e.g., cloud services), and support requirements. Many of these costs are not fully visible at the initial implementation stage but become measurable over time.
Within this framework, it becomes possible to estimate the full cost across key stages, including initial development or implementation, integration and scaling, ongoing maintenance and compliance, and future enhancements.
Corpsoft Solutions’ approach to telemedicine software development: combining cutting-edge expertise with swift project delivery
Our approach to telemedicine software development combines practical healthcare experience, strong technical expertise, and a focus on scalable, production-ready solutions. We understand that telemedicine platforms are not standalone products, but systems deeply integrated into clinical workflows, regulatory environments, and existing infrastructure.
Key pillars of our approach include:
- Dozens of healthcare-adjacent projects delivered. We bring hands-on experience from multiple healthcare and healthtech projects, allowing us to understand real-world workflows, common bottlenecks, and domain-specific requirements.
- Up-to-date compliance expertise. We design platforms aligned with current regulations, including HIPAA, GDPR, and relevant industry standards, ensuring systems remain secure, compliant, and audit-ready.
- Building for scalability from day one. Our architectures are designed to handle growing patient volumes, new service lines, and evolving product requirements without requiring costly rework or system redesign.
- Deep expertise in legacy system integrations. We specialize in connecting modern telemedicine platforms with existing EHRs, billing systems, and third-party tools, ensuring seamless interoperability and continuity of operations.
By combining these capabilities, we help healthcare organizations deliver telemedicine solutions that are not only functional but scalable, compliant, and built for long-term success.
Conclusion
Telemedicine software has evolved into a core component of modern healthcare delivery, requiring solutions that go far beyond basic video functionality. Successful platforms must support complex workflows, integrate seamlessly with existing systems, ensure compliance across multiple regulations, and deliver a high-quality user experience for both patients and providers.
At the same time, factors such as integration complexity, long-term cost of ownership, and scalability play a decisive role in platform success. Organizations that approach telemedicine as a strategic, long-term investment will be better positioned to deliver sustainable results.
Subscribe to our blog



